 The right renal artery was occluded, according to digital subtraction angiography (DSA). The patient was initially admitted to another hospital for flash pulmonary edema and deterioration of her previously medically controlled hypertension The patient was known with hypercoagulopathy (positive for Factor V G1691A (FV-Leiden) mutation) and single-functioning left kidney with previously treated stenotic left renal artery by balloon-expandable stent placement (12 months ago). Ī 39-year-old woman was emergently referred to our hospital with dyspnea, tachypnea, elevated serum creatinine and urea (9.7 mg/dl and 173.5 mg/dl respectively), and refractory hypertension (190/85 mmHg). Acute kidney ischemia is a medical emergency and should be treated immediately, as high rates of kidney loss have been reported in the literature after over 5 h of ischemia, despite revascularization. Positive outcomes following RAS have been reported in 96 to 100% of cases, with complications occurring in approximately 14%, including renal artery rupture/dissection, distal embolization, contrast-induced nephropathy, renal bleeding, and stent thrombosis leading to acute kidney ischemia (AKI). 
As the American Heart Association/American College of Cardiology (AHA/ACC) guidelines do not match utterly those of the European Society of Cardiology (ESC) considering the indications for percutaneous revascularization, the SCAI expert consensus concluded in 2014 that the candidates fit for renal artery stenting should present with cardiac disturbance syndromes, like flash pulmonary edema, as in our case, or acute coronary syndrome, hypertension resistant to medical treatment, not controlled by three or more medications at maximal doses, bilateral renal stenosis, or severe stenosis in a single-functioning kidney not controlled medically. 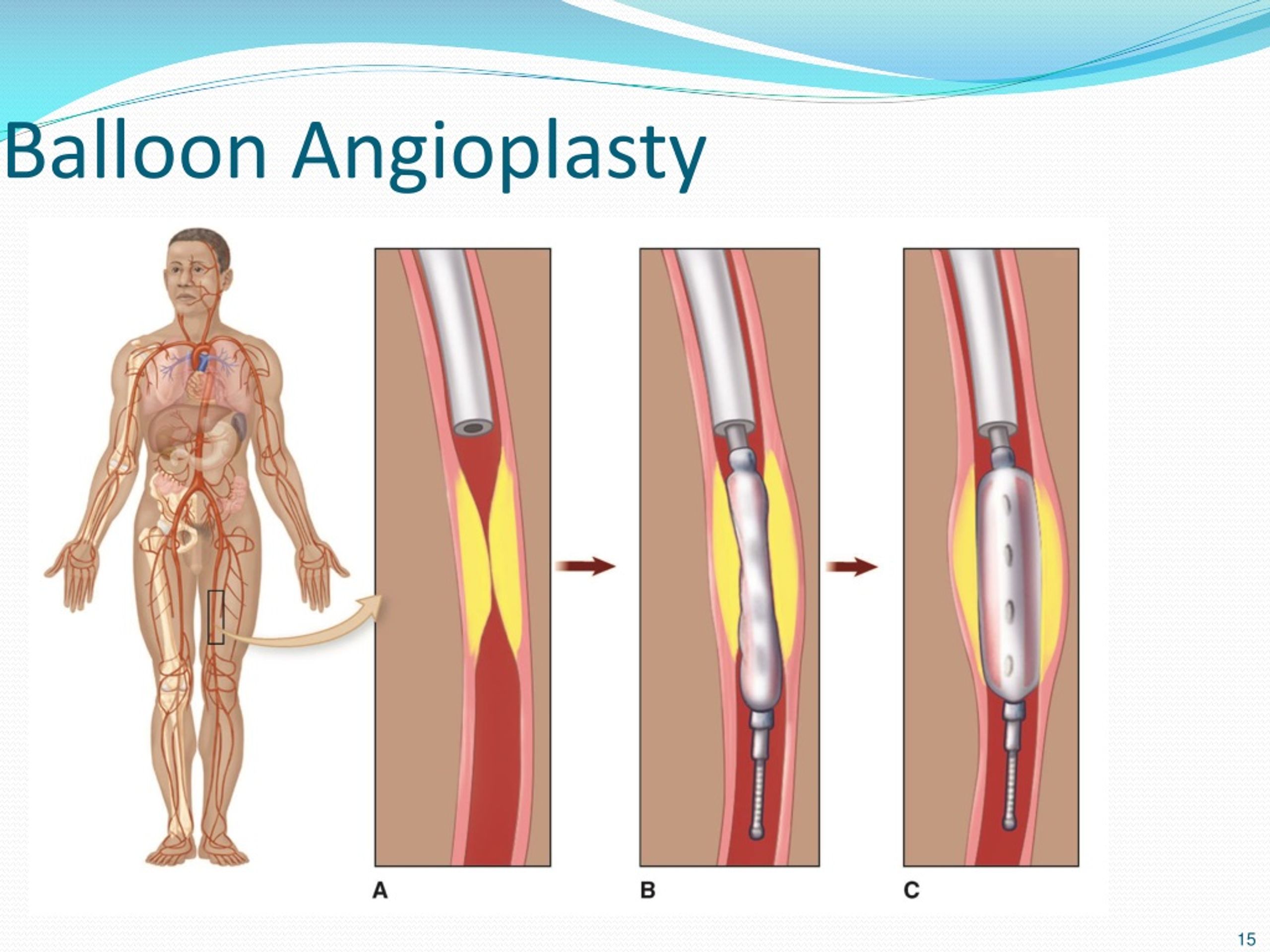
In the setting of renovascular hypertension (RVHT), anti-hypertensive drugs are indicated as initial treatment, while endovascular revascularization (RAS) is preserved for refractory cases, or as renal-salvage procedure in single-kidney cases with significant renal artery stenosis and deteriorating renal function. After 1 year of follow-up, the stent remains patent, and the patient is asymptomatic with stable renal function. The patient’s creatinine level decreased to 2.8 mg/dl at 12 days and to 1.5 mg/dl at 3 months. Ultra-selective, nephron-sparing coil embolization was successfully performed. Conclusionsįollowing more than 48 h of hypoperfusion of the left kidney, revascularization of the thrombosed RAS was successfully attempted with selective, trans-catheter thrombolysis, and balloon angioplasty. Periprocedural complications of guide-wire arterial perforation and reperfusion injury resulted in life-threatening hemorrhage. 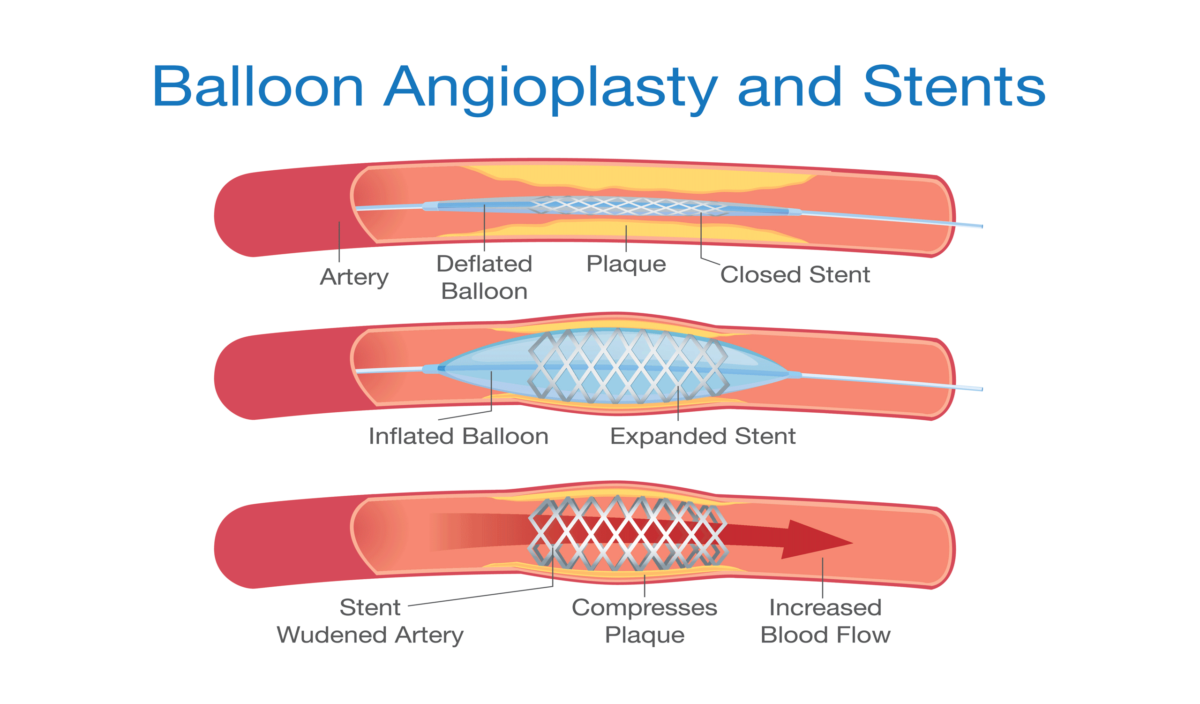
She was subsequently referred to our center for endovascular treatment of acute renal ischemia (AKI) due to RAS occlusion. 
Case presentationĪ 39-year-old woman with a single-functioning left kidney, previous left renal artery stenting (RAS), and known hypercoagulopathy was hospitalized for flash pulmonary edema, elevated serum creatinine (9.7 mg/dl), and refractory hypertension. The complexity of the case, including the rarefied simultaneous occurrence of complications-iatrogenic, as well as reperfusion injury, invite reporting and publication. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
